The Articulator as Standard Protocol for Orthodontic Diagnosis
In the orthodontic world, occlusal wear patterns on teeth are often a secondary consideration. In fact, they are valuable clues as to what is happening in the mouth. Consider the models in Figs 1a and 1b.
They are of a 25-year-old patient with a well- aligned Angle class 1 dentition following two years of full fixed appliance orthodontic treatment from 13 to 15 years of age. On completion of her orthodontic treatment, she wore a Hawley type retainer in the maxilla which was phased out over 18 months. In the mandible, a fixed canine to canine retainer was still in place.
Several years after the completion of the orthodontic treatment it became obvious that she was grinding her teeth at night. Equilibration of the dentition was first attempted in the hope of removing interferences. When this did not help, a mandibular full coverage orthotic for night time wear was made. She was still wearing this at night on an intermittent basis when I first saw her. The orthotic had been replaced several times due to her chewing through it, but it had failed to protect her from further deterioration of the dentition. There was no history or evidence of possible acid erosion of the teeth either from an extrinsic or intrinsic source.
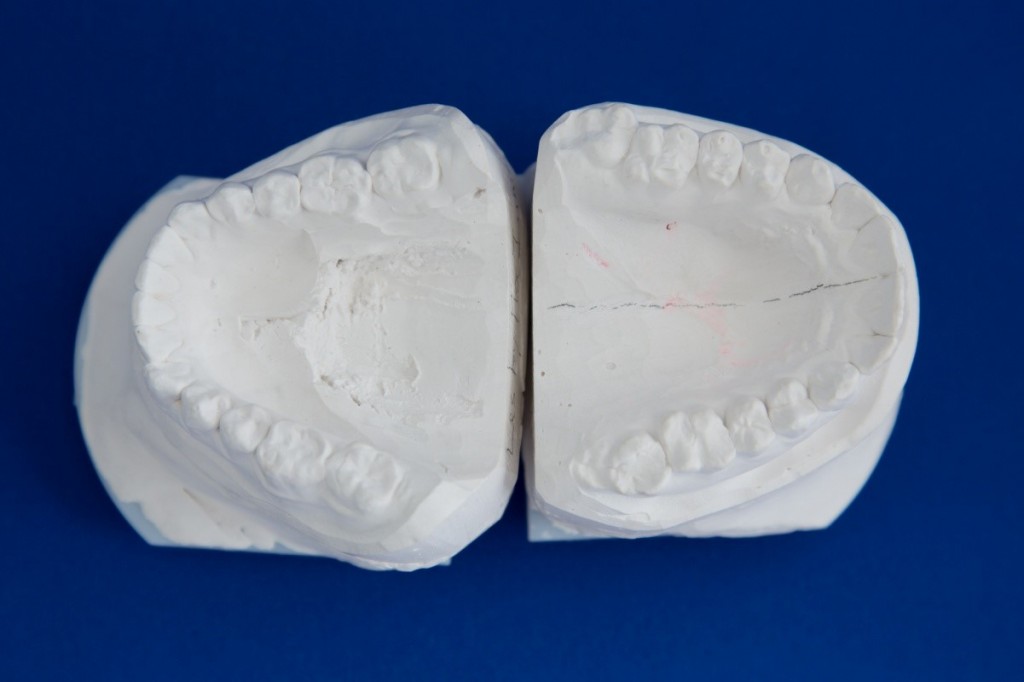
Fig. 2 shows the wear patterns on the occlusal surfaces of the molars. The loss of tooth material has been so severe that she had recently required root canal treatment on the mandibular left second molar.
From an appearance aspect, the patient has a very pleasing smile. The maxillary teeth have remained stable without the retainer. Despite the history of excessive grinding, she had few symptoms of TMJ dysfunction such as facial or joint discomfort, restriction of jaw movement, joint noise, headaches, etc. She was a healthy individual leading an active life, including various outdoor sports.
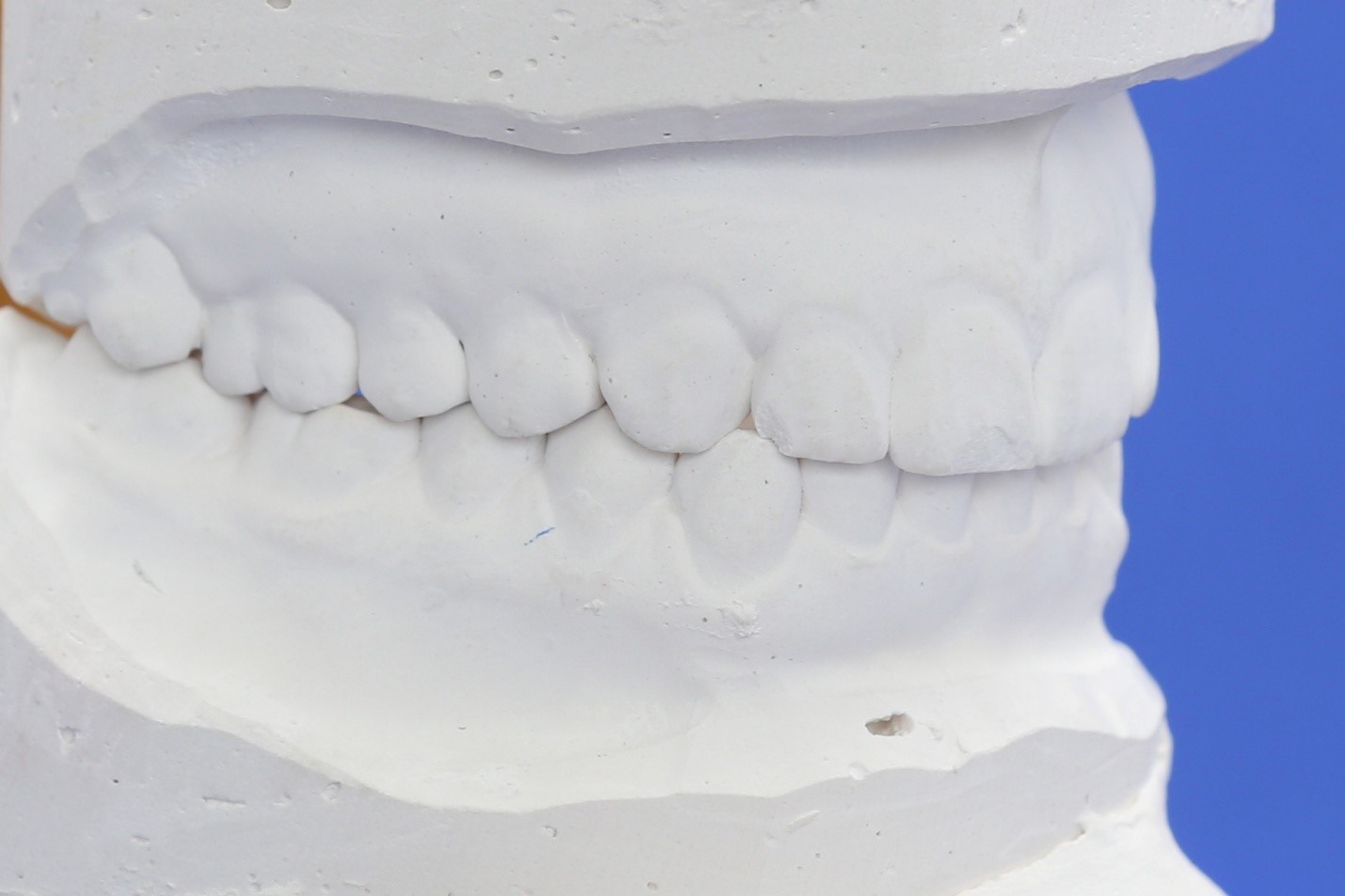
The heart of the problem becomes clear when the models are placed on an articulator, using a face bow mounting (Figs 3a, 3b). The bite registration for this was taken after several minutes of tooth separation with cotton rolls and before there was any occlusal contact. In this case, an Acculiner articulator is being used but other types of articulator with a face bow mounting are suitable.
The initial contact on closure in a centric path is on the left second molars. The patient has to fulcrum on the second molars and then the first molars to obtain full interdigitation of the teeth. The underlying biological force driving this is partly an attempt to level the lateral plane of occlusion which is canted up to the left.
The bruxing is also an effort to relieve a cranial displacement known a left torsion, by enhancing movement of the cranial bones. In particular, the action of the temporal and master muscles on the lateral aspects of the cranium causes the temporal bones to be moved laterally into flexion.
Understandably the orthodontist was happy with the aesthetic result he had achieved. When the patient first drew his attention to the night grinding, he attempted to solve this by equilibration of the teeth. When this did not work he resorted to an orthotic. However, when a patient requires root canal treatment because of bruxing, something is seriously out of balance. Without recognition of the underlying problems, further destruction of teeth is certain.
In my opinion, the use of a face bow and articulator plus a centric occlusal registration should be standard for all orthodontic patients as part of a diagnostic workup. Initially I only did this for adult patients but for many years have done so for everyone except youngsters under 5-6 years of age. In this particular case, mounting the models probably would have shown the maxillary cant. Suitable corrective steps could be taken to level the lateral plane of occlusion, accompanied by osteopathic adjustment to help relieve the cranial displacement.
Gavin


Leave a Reply
You must be logged in to post a comment.