A patient who chews gum seems an odd topic for a blog. After all, once the initial flavoring of the gum is lost there is nothing left but a piece of rubbery goo and the problem of getting rid of it in a discreet way. However to view gum-chewing purely as a social curiosity is to miss the physiological imperative underlying many so-called idle or parafunctional habits.
When I ask patients about chewing gum there is usually one of three possible answers. Patients with TMJ problems say that chewing gum was one of the first things they learned to avoid. A malfunctioning TM joint can suddenly become uncomfortable or acutely painful due to the extra load placed on the joints.
The other two groups are gum enthusiasts. One group chews it as much as possible even when this is not socially acceptable. They do not have painful TM joints but the constant muscle contraction helps remove the lactic acid build-up in the masticatory muscles. There may well be some form of orofacial malfunction but the joints are not a primary source of pain.
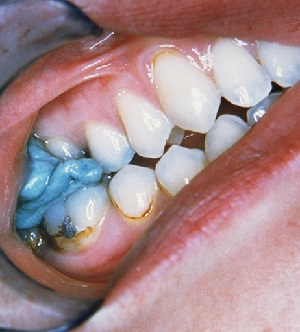
The final group is the most intriguing from a diagnostic aspect. These patients are usually quite aware of what they are doing and tend to carry a packet of gum with them throughout the day. They quickly chew through the outer hard coating then wedge the gum between the two arches of teeth Fig 1. The gum is left there for extended periods, acting as a makeshift orthotic. It is unobtrusive and gives temporary stability to the mandible. Patients will work out for themselves whether they need one, two or even more pieces to acquire a satisfactory mandibular prop.
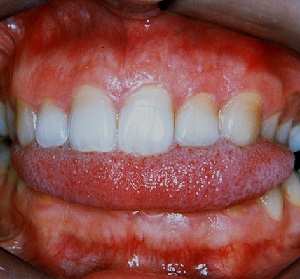
The patient in Figs 2-5 shows a combination of behaviors. She readily described how she experimented until she found several ways of rescuing herself from considerable TM joint discomfort. Her Angle description is of a unilateral left-sided Class 11 malocclusion with a marked deviation to the left on mandibular closure and a crossbite of the left posterior quadrants. The osteopathic description is a left sidebend displacement of the cranial and facial features (Fig 2). This has been described in the two articles on sidebend by Dr. Dennis Strokon and myself and is available on this web site.
For this patient, the tongue was the most convenient short-term solution to support a temporary shift of the mandible to a more centered position, either with an anterior resting position Fig 3 or a left shift to cushion the mandible Fig 4. The patient showed considerable ingenuity by working out how to use chewing gum as a more discreet longer-acting device Fig 5. She reported that the gum was the most practical solution in her everyday routine and was rarely without it.
Once again, as with the hockey player in the previous blog, the subconscious self-regulating mechanisms of the body will attempt to solve a biological imbalance. In this case the patient herself consciously worked out an oral solution. It makes good sense for us to take thorough case history notes, study the “wisdom of the body” and incorporate this information into our treatment planning.
Gavin





Leave a Reply
You must be logged in to post a comment.