 Even the most junior detective knows a strong case can hinge on the collection and preservation of evidence. Detectives know that following well-established procedures is the only way to capture vital information at a time when the information has not yet revealed itself to be of importance to the case.
Even the most junior detective knows a strong case can hinge on the collection and preservation of evidence. Detectives know that following well-established procedures is the only way to capture vital information at a time when the information has not yet revealed itself to be of importance to the case.
So it is with the collection of orthodontic diagnostic evidence—in particular from study models. Unfortunately, common clinical practices destroy valuable information that could otherwise tip the balance toward a more successful outcome. This helpful evidence is literally ground into dust.
Study models have always been an important diagnostic tool in orthodontics. An informal survey of my orthodontic colleagues suggests that while digital models can be helpful, plaster models which have been bench–articulated, with the teeth in habitual occlusion, are still generally accepted as a starting point in diagnosis.

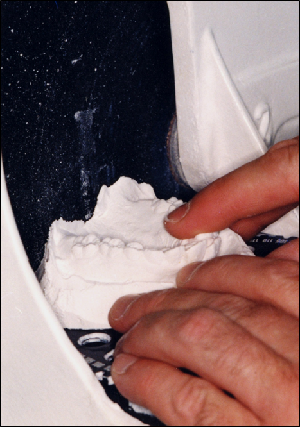
Fig 1 shows a maxillary plaster cast about to be moved forward against the grinding wheel of the model trimmer. The technician holds the model against the vertical guide plate, with the occlusal surfaces of the teeth resting on the soft spongy material of the guide plate to avoid fracture of the teeth. This first grinding or “cut” establishes the base of the maxillary model. The remaining cuts to the maxillary cast are influenced by this initial grinding (Fig 2).
Let’s assume that the patient has a cant (angular deviation) of the lateral plane of occlusion up to one side. The effect of the very first cut is to parallel the maxillary model base with the cant of the occlusal plane, effectively wiping out the primary physical evidence of the cant. Of course, other clues that there is a cant may remain; it may still appear on a full-face photo or on a posteroanterior radiograph if one is included in standard records. In cases where the cant of the mouth is obvious, this deviation may be noted, but in cases where the cant is mild, it may be dismissed as irrelevant or it may be completely overlooked.
Tying in the lateral cant of the maxilla to the facial and cranial features is not part of a conventional diagnosis. But practitioners who do, have precious evidence in their hands that can help shape more effective treatment plans. The trimming of the mandibular model is usually done by relating it to the maxillary model and using the maxillary model as a guide to the cuts on the mandibular cast. To do so, the teeth are put into habitual occlusion. This is accepted orthodontic procedure unless there is a TMJ problem in which case an articulator, face bow and centric relation bite registration may be preferred. Many years ago I started to use this more elaborate protocol for all patients except the under 10 year-olds. It is a source of valuable information, especially from a functional aspect. Now when I am handed a set of bench-trimmed models and asked for an opinion I realize how much more information is needed to give an adequate answer.
What is apparent is that by modifying common procedures, we can take advantage of information not previously considered relevant.
Gavin

Leave a Reply
You must be logged in to post a comment.